While COVID-19 symptoms are often temporary, some individuals endure long-term effects. This article describes some of the most common symptoms of long COVID-19, briefly examines the possible causes, and then delves into dietary approaches to support long COVID-19 recovery.
How Is Long Covid Defined?
Long Covid continues to be a hidden epidemic in many ways.
Sometimes referred to as long-tail Covid, post-Covid, or long-haul Covid is a disorder in which individuals display symptoms for more than twelve weeks following an infection with Covid-19 that cannot be explained by another explanation.
According to the Department of Health and Social Care a third of Covid-19 patients continue to have symptoms after twelve weeks. According to one of the largest government-funded COVID-19 studies to date, approximately 2 million individuals in England are expected to experience long-term consequences after being infected with COVID-19.
Long Covid is not an unusual occurrence; post-viral syndrome can occur following recovery from a number of viral illnesses, including the common cold, influenza, pneumonia, Epstein-Barr virus, SARS, and HIV.
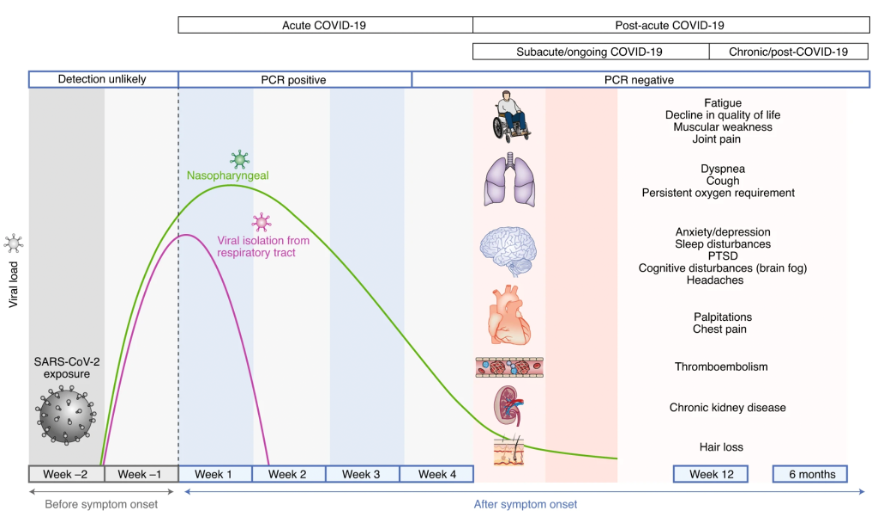
What Are Long Covid’s Signs and Symptoms?
Post-acute COVID’ is a broad term that refers to a variety of incapacitating symptoms. COVID-19 has been linked to over 50 long-term adverse effects in studies. The following are the most often reported symptoms:
- Fatigue
- Headache
- Chest discomfort or constriction
- Memory and concentration issues (“brain fog”)
- Inability to sleep (insomnia)
- Palpitations of the heart
- Dizziness
- Needles and pins
- Joint discomfort
- Anxiety and depression
- Ringing in the ears, earache
- Nausea, diarrhoea, stomach pains, and appetite loss
- Fever, cough, headaches, sore throat, or an alteration in one’s sense of smell or taste
- Rashes
These symptoms commonly resemble those of rheumatic diseases such as rheumatoid arthritis, autoimmune disorders, and others such as fibromyalgia and chronic fatigue syndrome, all of which are characterised by swelling, hyper- and/or autoimmunity, and some, such as chronic fatigue, are associated with viral persistence following acute infection with pathogens such as Epstein Barr virus (EBV) and Human Cytomegalovirus (CMV).
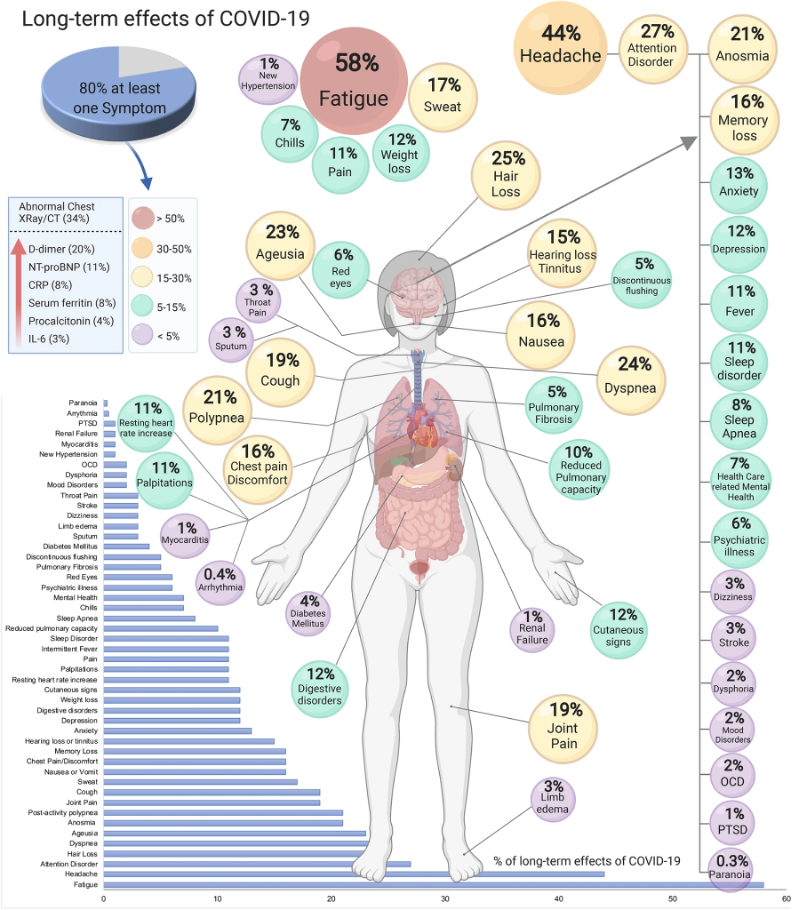
What Is The Cause Of Long Covid?
According to research, many individuals with prolonged COVID experience difficulty with many organs, showing that the disorder is multisystemic. Given the widespread expression of the SARS-CoV-2 entry receptor ACE2 in multiple organs, the occurrence of multiorgan disorders is unsurprising.
Given its novelty, the response to long COVID-19 is still in its infancy. Despite extensive examination of the several symptoms of long COVID, no clear explanation for the underlying process of long COVID-19 exists, and much remains unanswered.
Numerous and disparate causes may contribute to long-covid symptoms. Organ damage caused by an exaggerated inflammatory response induced by the virus, persistent reservoirs of SARS-CoV-2 in some tissues that could result in post-infection morbidity, pathogen reactivation due to immune dysregulation, host-microbiome changes, clotting/coagulation problems, and autoimmunity induced by molecular mimicry among SARS-CoV-2 and self-proteins have all been hypothesized to play a role.
A nutritional therapy approach to long-Covid
The conventional western diet (rich in saturated fat, processed carbs and sweets, deficient in fibre, unsaturated fat, and antioxidants) has been proven to have an effect on the adaptive immune system (second line, delayed defence against infection), dampening its activity. On the other hand, there is now evidence that some lifestyle and environmental factors can act as immunoadjuvants and significantly impact a person’s response to a viral infection. The following mechanisms may be involved in the ability of food-derived compounds to reduce viral infection and severity.
Improve metabolic health
Obesity and compromised metabolic health, such as hyperglycemia, hypertension, and subclinical inflammation, are linked to an increased risk of severe and long-term COVID-19. It’s important to understand that not only obese people are metabolically unhealthy, in fact, 20% of people considered “lean” are metabolically unhealthy. A nutritional approach can support metabolic health in multiple ways. A foundational approach would be to manage blood sugar response to avoid energy fluctuations across the day. Here are some simple strategies to reduce blood sugar spikes:
- Aim to have a good source of protein at every meal, such as oily fish, lean meat, legumes and pulses.
- Prefer complex carbohydrates sources such as peas, beans, whole grains, and vegetables instead of refined options.
- Avoid excessive sugar consumption, including options perceived as ‘healthy’ such as agave syrup.
- Prefer low glycemic foods.
A more comprehensive approach, targeted to each individual needs and lifestyle factors, might be required to establish optimal metabolical health.
Balance inflammatory pathways
When we’re feeling down, it’s easy to grab comfort foods, often processed and heavy in fat, sugar, and salt. However, for people recuperating from a viral illness, it is crucial to stock up on key nutrients to assist reduce inflammation and to stick to basic, unprocessed meals that will not worsen any post-viral inflammation. A personalised dietary intervention based on nutrient-dense foods and anti-inflammatory and antioxidant principles can help to reduce inflammation, commonly seen in post-viral cases. Following an antioxidant-rich diet, such as the Mediterranean diet, which includes fatty fish high in omega-3, olive oil, and a variety of vegetables and pulses, can be an excellent first step toward lowering neurological and systemic inflammation after infection. It is also vital to consume nutrients that support energy production and mitochondrial health (our cells’ powerhouse’), such as B vitamins (found in eggs, fish, meat, dark leafy greens), magnesium (found in pumpkin seeds, spinach, avocado) Coq10 (found in organ meats, fatty fish, beef).
There are similarities between Chronic Fatigue Syndrome (CFS) and Long Covid; there are also similarities with histamine intolerance and Mast Cell Activation Syndrome (MCAS) and Long Covid too. Histamine levels can rise after a viral infection, and in some people, this can trigger an allergic reaction in the body, resulting in symptoms such as headaches, IBS, chronic tiredness, sinusitis, and shortness of breath. This might imply that a low-histamine diet could help lower the severity of Long Covid symptoms. However, although some case reports show positive outcomes, there is currently a dearth of evidence that reduced histamine diets help control inflammation in chronic COVID-19 patients. Furthermore, if not followed under the direction of a certified practitioner, a low histamine diet can be restrictive, difficult to follow and lacking in nutrients leading to nutritional deficiencies.
Reduce oxidative stress and increase antioxidant levels
Vitamins (A, B, C and E) and trace minerals (e.g. selenium, zinc, magnesium, iron) are recognised to help support the immune system. These are best obtained through a varied whole foods diet, which includes:
● Fish, especially oily fish – high in omega-3, iodine, B6, B12.
● Meat – an excellent source of zinc, iron and B vitamins.
● Leafy greens – high in vitamin C, folate, vitamin A.
● Nuts and seeds – high in vitamin E, selenium, and magnesium.
● Fruits – high in vitamin A, vitamin C and many other antioxidants.
Eating a diverse and colourful range of vegetables is especially important for optimal recovery. They are rich in fibre and polyphenols, which have been linked to a reduction in inflammatory comorbidities. Cruciferous vegetables, such as broccoli, cauliflower, and rocket, can aid in the production of the master antioxidant glutathione, making them an important type of vegetable to consume on a regular basis.
Harmonise gut microbiome
The microbiome (microbes that live in your gut) play an important part in maintaining the immune system, supporting overall health, having disease-modifying potential. Studies propose a direct interaction between the gut microbiome and COVID-19, showing that the microbiome appears to influence the course and severity of COVID-19.
Several studies have also found that SARS-CoV-2 infection causes alterations in the microbiome. These changes can occur as a result of a direct infection in the gut, as a result of increased inflammation and interaction between the oral, lung, and gut microbiome. If dysbiosis (imbalances) in the microbiome develops, it can cause or exacerbate inflammation, increase intestinal permeability, and alter the balance of signalling metabolites. Some of the long COVID-19 symptoms, such as fatigue, poor sleep, joint pain, anxiety/depression, headache, and diarrhoea, have also been linked to gut microbiome imbalances.
You may improve the diversity of your microbiome by consuming a variety of plant-based, high-fibre meals and eliminating ultra-processed and junk food. Following a Mediterranean diet can promote gut microbiome variety and reduce inflammation, perhaps putting you in a better position to fight viruses like coronavirus. Additionally, you may benefit your microbiome by consuming probiotic-rich foods such as natural yoghurt, kefir (fermented milk), kombucha (fermented tea), and fermented vegetables, all of which contain live bacteria. COVID-19 infection has also been demonstrated to damage the gut epithelial barrier, allowing bacteria to migrate through the epithelial cells into the systemic blood vessels, inducing additional inflammation. Therefore, restoring gut function should consequently include a focus on gut epithelial health.
How can I help to support your Long-Covid journey?
I can offer a rehabilitation programme to individuals suffering from Long Covid. Because the virus may impair any organ and the individual’s mental health, this will be a comprehensive program tailored to each individual’s needs. During our initial 90 minutes consultation, I will assess your current symptoms, taking your personal and family medical history into account. We will discuss in detail your current nutrition and lifestyle choices and how covid has impacted your health. Based on this initial input, I will define a tailored nutritional and lifestyle plan. If relevant, recommend health tests to inform my assessment and the nutritional plan and high-quality practitioner-grade supplements.
If you would like to discuss your case in more detail and see if we could work together, schedule a complimentary discovery call.


 5 Habits for a Great Start to Your Day
5 Habits for a Great Start to Your Day
Leave a Reply